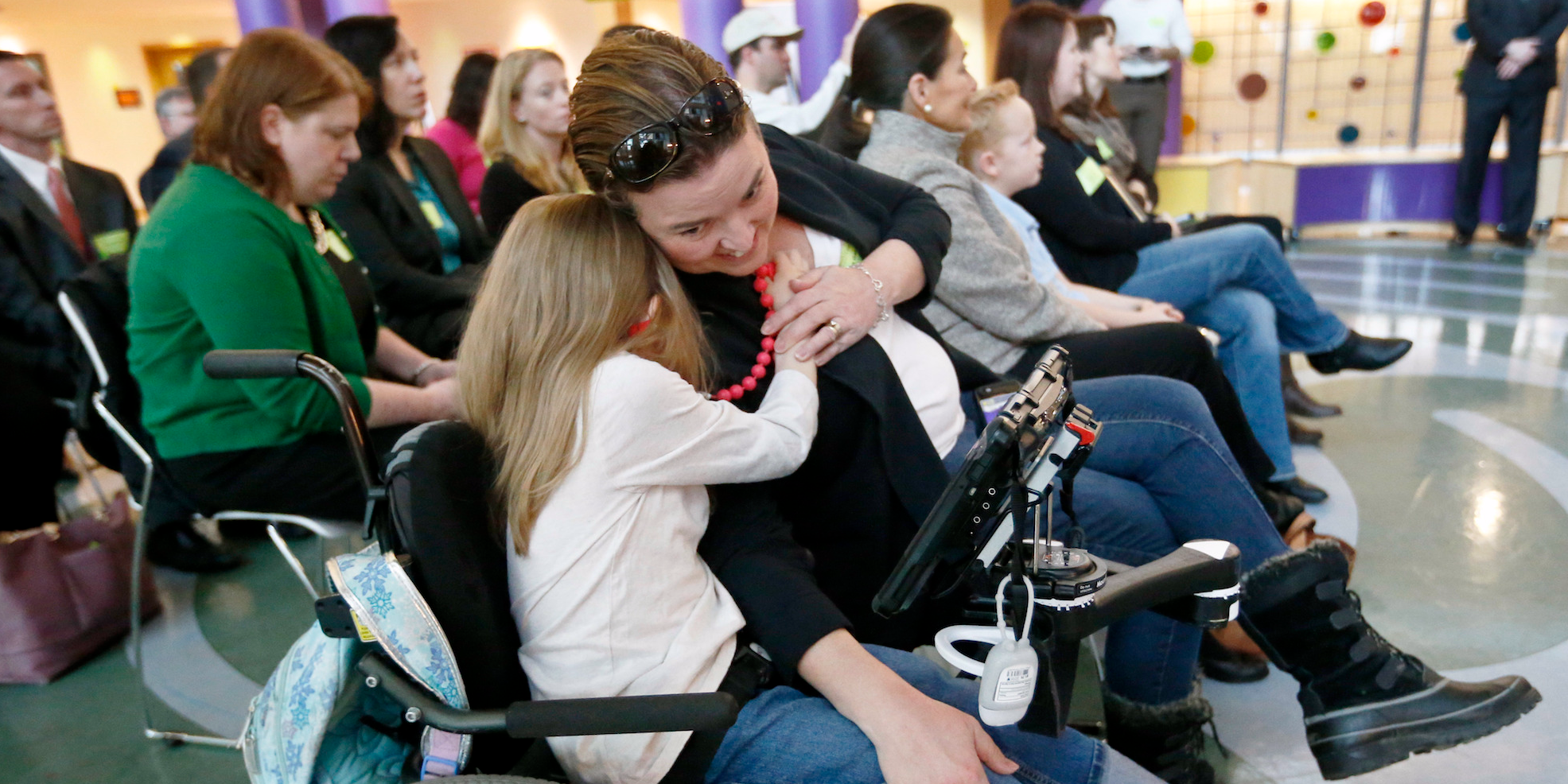- If Congress doesn’t reauthorize longterm funding for the Children’s Health Insurance Program (CHIP), millions of children could lose health care coverage.
- A handful of states are expected to run out of money in the coming months.
- Medical officials in those states are already sending out termination notices, warning families that plans could be canceled.
- Even if Congress does eventually restore CHIP money, the delay in funding will have already cost taxpayers hundreds of thousands of dollars.
Health insurance for millions of children is still on the line as Congress remains divided over how to fund the Children’s Health Insurance Program (CHIP), a crucial government program that has provided healthcare to millions of Americans and helped to drastically reduce the uninsured rate of children since its implementation in 1997.
Before breaking for the holiday recess month, Congress passed a short-term funding measure that allocated close to $3 billion to CHIP. It’s estimated that this additional funding will allow the program to run through March.
“This alleged extension until March doesn’t cut it as states freeze enrollment & send out letters warning that coverage will end,” former Democratic presidential candidate Hillary Clinton tweeted on Tuesday. “This is frightening to parents & wreaks havoc for states.”
“Enough is enough,” added Clinton, who played a significant role in getting CHIP passed back in the ’90s while serving as first lady.
A lack of long-term funding could result in roughly 2 million children losing coverage and becoming uninsured, according to a recent report from Georgetown University's Center for Children and Families.
"These are families making $8, $10, or $12 an hour that don't have insurance. And they're going to get letters saying 'your insurance is canceled,'" Ohio Sen. Sherrod Brown said during a debate on the Senate floor November 30. "How can we let that happen?"
The reauthorization deadline for CHIP passed September 30 without Congress agreeing to an extension, making it the longest lapse in funding since the program was first introduced.
"The politics are ugly. This should not be a Republican or Democratic issue," Colorado Lt. Gov. Donna Lynne told Business Insider. "There's never been any talk of it not making sense."
"I feel like there's a little hostage taking with kids and pregnant women in the middle," she added.
Time is running out

Now that Congress is back in session after the holiday recess, CHIP proponents are holding out hope that both parties can come together to secure a 5-year funding extension.
Such a move would be the quickest way to end concerns families may have about the future of their coverage, said Tricia Brooks, a healthcare policy expert and former CHIP director for New Hampshire.
"We are guardedly hopeful because unlike all of the other health policy initiatives Congress has tackled this year, CHIP actually has bipartisan agreement in the House and Senate," Brooks told Business Insider.
"The fact that states had leftover funds and that there was emergency money distributed to states gave Congress the feeling that were wasn't as much urgency," she added. "But that cushion is getting extremely thin. Congress needs to act."
The only other time Congress failed to reauthorize it was in 2007, when then-President George W. Bush vetoed reauthorization because he believed the Democrats' proposal to spend billions more on the program would encourage families to leave the private insurance market. After just five days, lawmakers compromised and funding was quickly reissued.
Today's gap in funding has forced states around the country to rely on leftover funds and emergency government grants to maintain coverage for the millions of people who might otherwise be uninsured. But those temporary funds are quickly disappearing.
"We're concerned about the cost to the people and the magnitude of the anxiety it is producing," Lynne said. "Imagine if you're a pregnant woman and you're going to lose your insurance?"
'We don't have any money anymore'

CHIP itself is not controversial. It has wide bipartisan support as Brooks says.
But exactly how the annual $15.6 billion program should be paid for is the issue under dispute.
Republicans have proposed cutting back the Affordable Care Act to pay for CHIP while Democrats have proposed tying the program's reauthorization in with measures to stabilize the law, more commonly known as Obamacare.
"We're going to do CHIP. There's no doubt about it in my mind, " said Sen. Orin Hatch of Utah, who helped craft the program with Sen. Ed Kennedy of Massachusetts in the 1990s. "But the reason CHIP is having trouble is because we don't have any money anymore."
CHIP currently provides health insurance for roughly 9 million children nationwide who come from families with incomes just above Medicaid eligibility levels.
The program also includes coverage for more than 327,000 pregnant women through the "unborn child option." Technically, these recipients are classified as children even though the women are the ones who are actually being treated.
How states can respond to a loss of federal funds depends on how they implemented CHIP in the first place.
For states that used the money to expand Medicaid to insure more children, they will still have to cover those recipients, albeit with some other source of funding, even if the government no longer helps.
For states that created separate CHIP programs, those recipients are likely to lose coverage completely, or at best, receive more expensive coverage through employer-sponsored or marketplace exchange alternatives if their families can afford those options.
Some states have a combination of CHIP-funded Medicaid expansion and separate CHIP programs, complicating the situation even further.
States plan emergency measures
Late night host Jimmy Kimmel brought his newborn son on stage in December to make an emotional plea for Congress to restore CHIP funding.
"Now CHIP - [it] has become a bargaining chip," Kimmel said, cradling his son Billy, who received life-saving open heart surgery just hours after birth earlier this year.
"It's on the back burner while they work out the new tax plans," he continued. "Parents of children with cancer, diabetes and heart problems are about to get letters saying their coverage could be cut off next month. Merry Christmas, right?"
A handful of states are on the brink of running out of money, some as soon as next month.
Carrie Williams, a spokesperson for Texas' Health and Human Services Commission, told Business Insider last month that without Congressional action, the Lone Star State would be forced to end CHIP coverage by February 1 for more than 450,000 children.
But on December 15, the Centers for Medicare and Medicaid Services, which administers CHIP, guaranteed Texas $135 million in funds to continue coverage until March.
Under state law, HHSC must notify families that their plans are being canceled at least 30 days before termination.
Texas' situation is especially dire because of the damage caused by Hurricane Harvey. After the disaster struck, the government waived co-pays and enrollment fees for CHIP recipients. That meant the state would be collecting less money, which is why they're relying on the federal government for additional grants. Texas has the most CHIP recipients in the country after California.
Other states continue to weigh their options in light of the roughly $3 billion in funding Congress allocated to states last month.
Officials overseeing the West Virginia Children's Health Insurance Program (WVCHIP) have gone so far as to already approve a plan to close its program - which covers 21,321 children - by February 28.
But the plan won't be finalized until the program's board members know how much of the $3 billion in funding the state will receive. For now, West Virginia's Department of Health and Human Resources will delay sending termination notifications to families and providers, according to communications director Allison Adler.
'We've never had to do this before'
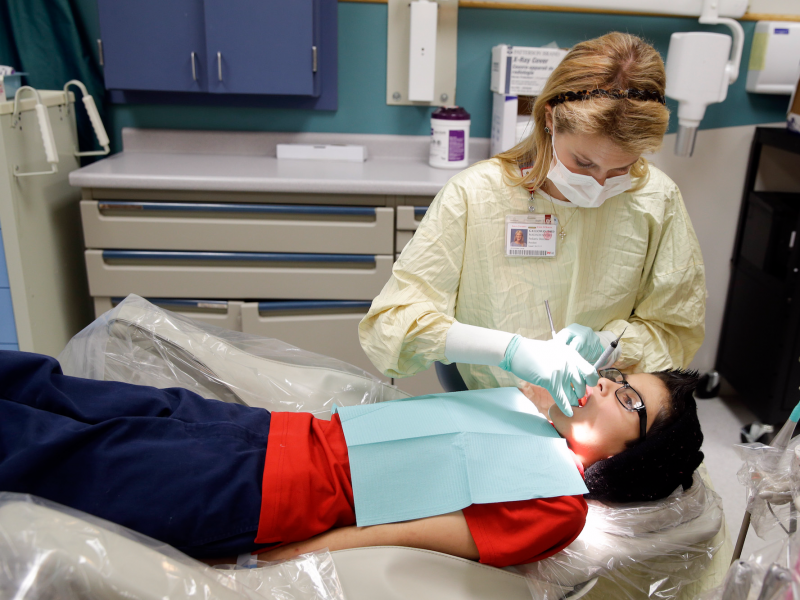
The longer Congress delays funding, the more states like West Virginia will prepare contingency plans in the event that money is not restored.
But it's hard for medical officials to gauge exactly when they should take action - such as sending out notice letters to families and doubling up on call center staffing for the inevitable barrage of inquiries - since they have to rely on Congress to make the next move.
"They [states] are trying to hold off on taking action as long as possible because they don't want to cause concern among families," Samantha Artigo, an analyst at the Kaiser Family Foundation, told Business Insider. "But as we get further along, they are really going to be bumping up against difficult deadlines where they will need to begin taking action. It cannot be done overnight."
Medical officials in Colorado have already sent notice letters to the families of the roughly 75,000 children and 800 pregnant women who might lose coverage in that state. Last month, state lawmakers approved a $9.6 million stopgap measure to allow CHIP to survive an extra month, according to The Denver Post. Previous estimates predicted coverage would end January 31.
Shelisha Coleman, a spokesperson for Florida's Agency for Health Care Administration, told Business Insider in December that the state had enough funding to last until the beginning of February. The healthcare of 198,605 children in Florida is on the line.
On December 1, Nevada received a nearly $5.6 million grant to provide coverage through the end of the year and into the new year. Utah also warned recipients that it will exhaust funds by the end of of this month.
The Department of Social Services in Connecticut announced that it has enough money to last through February 28. Officials in Virginia and Pennsylvania began notifying families last month that they could lose coverage if Congress continues to stall.
"We've never had to do this before," Linda Nablo, an official with Virginia's Department of Medical Assistant Services, told Kaiser Health News. "How do you write the very best letter saying, 'Your child might lose coverage, but it's not certain yet. But in the meantime, these are some things you need to think about'?"
Families are preparing, too.
Myra Gregory is the mother of 11-year-old Roland, who has a rare form of lung cancer. In November, Gregory wrote an op-ed in the St. Louis Post-Dispatch asking Congress to get its act together.
"If Congress forces Missouri to drop Roland's coverage, our family will be in an impossible situation. I don't have the savings to pay for Roland's care out of pocket," Gregory said. "I don't have family and friends - much less a bank - who will loan us tens of thousands of dollars for Roland's treatment."
Gregory created a GoFundMe page to raise money for her son.
A lose-lose for the taxpayer

The kicker is that states will still lose money even if Congress restores funding.
Writing, printing, and mailing termination notices to families requires time and money. So does notifying insurance providers and other stakeholders, submitting paperwork to the CMS, and paying call center staff overtime for helping concerned parents figure out how to proceed in the absence of CHIP.
A Georgetown University study estimated that ending CHIP will cost Colorado, for example, at least $300,000.
"Inaction by Congress costs states time and money as officials grapple with various 'what if' scenarios," the study's authors wrote.
In early November, the House passed a bill that would provide funding for CHIP for five years. That bill stalled in the Senate. Subsequent proposals, meanwhile, have been few and far between, leaving state budgets in limbo and families fearing the worst.
"There's no question that if CHIP isn't refunded, we're going to do a turn on the success in covering children that we've had," said Brooks, the healthcare expert. "Where are the values in this country?"