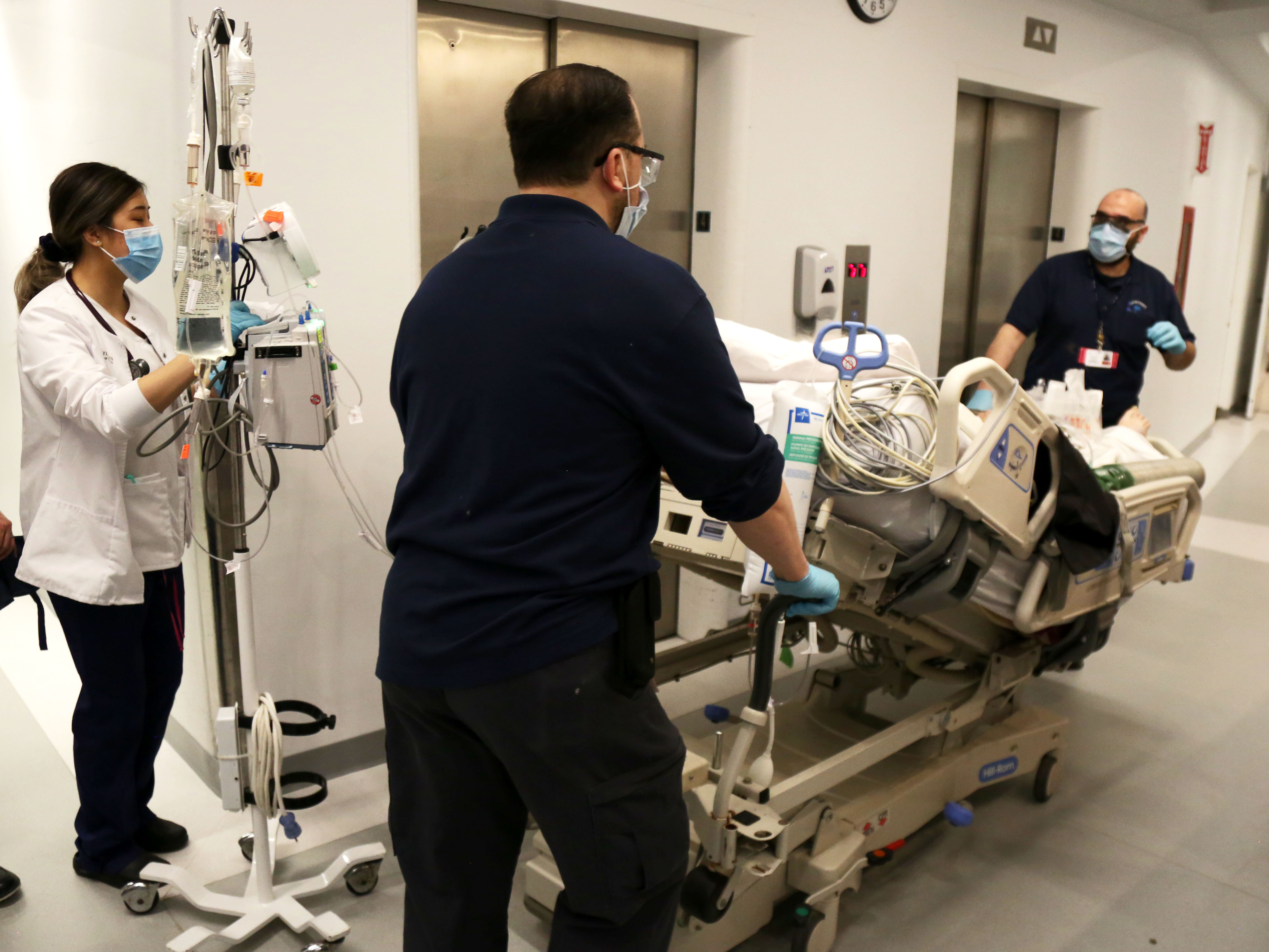
- New York City’s hospitals are getting overwhelmed with coronavirus patients, already filling hospital beds across the city and putting strain on frontline workers.
- As of Wednesday, Brooklyn had 12,076 confirmed cases of the novel coronavirus, up from 4,400 cases the week before.
- The pandemic has transformed everyday life at Maimonides Medical Center in Brooklyn.
- Dr. Patrick Borgen, the chair of surgery at the hospital, said that on Tuesday morning, he counted five codes go out over the speakers in a matter of hours. Before the pandemic, a call for a rapid response to revive a patient might happen every few days, he said.
- Visit Business Insider’s homepage for more stories.
Dr. Patrick Borgen’s hardest day so far in the pandemic was Friday, March 27.
Borgen’s the chair of surgery at Maimonides Medical Center in Brooklyn’s Borough Park neighborhood. That day, he was helping move patients onto a floor that was typically used for recovery by people who had routine surgeries like gall bladder and appendix removals. Those patients tended to get on the mend quickly.
Now, however, the patients occupying the beds were there because of the novel coronavirus. They were “unbelievably sick,” Borgen said, and a number of them would not get better. Now, too, there was an additional weight on the staff.
“What was really palpable was that the healthcare team was also at risk,” Borgen said. That day, the hospital also had several patient deaths. “That kind of thing is just devastating to the healthcare team.”
Even so, he said, the team managed to come to work the next day.
The hospital has transformed as part of its "wartime" response to the coronavirus pandemic, compared to what it was like before the outbreak began.
For instance, on Tuesday morning, Borgen counted the number of announcements that patients were coding. That is, instances in which patients suddenly deteriorates to the point where breathing stops, heart rates drop and healthcare workers have to rapidly respond to the situation to revive the patient.
In peacetime, there's a code maybe every few days. The frequency now, is much higher.
"In a couple hours there were five codes," Borgen said.
Never miss out on healthcare news. Subscribe to Dispensed, our weekly newsletter on pharma, biotech, and healthcare.
What it's been like to treat patients
As of Wednesday, New York City had nearly 45,000 positive coronavirus cases, of which 12,076 were in Brooklyn - up from 4,400 the prior Wednesday.
The hospital has felt the influx of seriously ill patients. Maimonides now has hundreds of COVID-19-positive patients, up from just dozens a week ago, Borgen said.
The active cases of COVID-19 patients have been doubling every three to four days, Borgen said. While the hospital has been able to discharge about 100 patients, the rate of new cases being admitted far outpaces it. The hospital is currently up to 150 intensive care beds, up from the 60 it regularly operates. Borgen said the hospital's anticipating it'll eventually need 400 ICU beds on hand.
"We're still very worried about the next two weeks look like," Borgen said.
The high volume isn't the only aspect putting strain on hospitals. Borgen recalled going through his training in the 1980s as the HIV/AIDS crisis hit. While the virus was new and doctors didn't know how to treat it, patients typically deteriorated over a longer period of time.
"With this disease, when you get the bad form, the downhill is extremely dramatic and extremely fast," Borgen said.
To date, New York City has reported 1,139 deaths associated with the novel coronavirus.
As a cancer doctor, the reality of patient deaths isn't new to Borgen. Typically, if there's a death, he has time to process it.
"This would be like losing 15 cancer patients a day," Borgen said. Everything is different.
Lessons to the rest of the country
New York City has emerged as an early center of the outbreak following Seattle, but other places in the country stand to be hit hard as well as the virus spreads.
"Our knowledge of this virus is about three months old," Borgen said. "We're learning as we go the quirks and the eccentricities and the scary things that this virus can do."
For instance, within the last week the hospital has changed its approach to using oxygen on patients who are having trouble breathing.
Now, instead of progressing quickly to ventilators, the organization is relying more on high flow oxygen therapy, with the hope that by keeping patients breathing on their own and able to move, they might be able to recruit extra airways that were otherwise blocked by the virus.
To be sure, Borgen said, it's not because the organization is running low on ventilators.
"This is not because of equipment shortages," Borgen said. "Once someone gets on a breathing tube it's a rocky course."
It's also meant that other parts of the country have yet to be hit as hard in the initial weeks of the outbreak in the US. Borgen said that on a webinar with cancer doctors from around the country, many had trouble believing it could get as overwhelming as it has for New York City. He gets it.
"Until I saw this, I couldn't believe it," Borgen said.
But, he said, it's important to take this pandemic seriously and get prepared. That includes getting resources like personal protective equipment and ventilators on hand now - about quadruple what one might think is needed.
"Now's the time to find sources for those services," Borgen said.
Do you work at a hospital? Business Insider would like to hear what you're seeing on the front lines of the coronavirus response. Contact the author at [email protected].