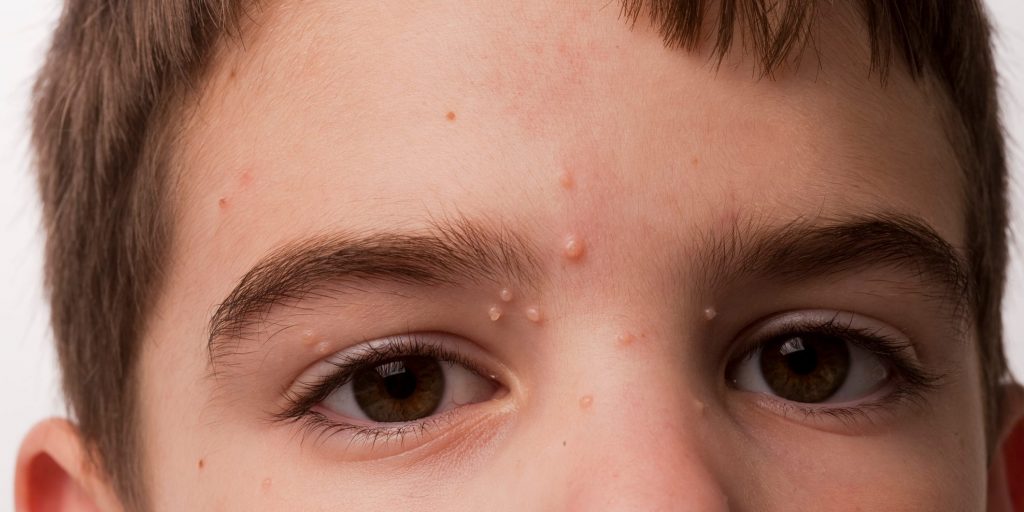
- Molluscum contagiosum, a common skin infection, causes small, painless bumps that can last months.
- It’s mostly harmless but can be easily transmitted through shared items, touch, or sexual activity.
- Your body will eventually clear the infection, but treatment from a dermatologist can speed this up.
Molluscum contagiosum is a contagious but common skin infection that can be transmitted through touch or shared items like towels, clothes, or gym mats. While it's mostly found in children, adults can also acquire this infection.
The infection causes firm but painless bumps, called lesions, that usually go away on their own within 6 months to 2 years. However, scratching these lesions can cause scarring or bacterial infections that may need treatment – especially if you have a weakened immune system.
Here's what you should know about molluscum contagiosum.
Stages
"It usually starts with a raised small bump that can be flesh-colored. Over a few weeks, you may see more of these lesions, and bumps may get bigger," says Dr. Loretta Cody, a pediatrician in private practice.
Here's a breakdown of how molluscum contagiosum progresses:
1. First appearance
Bumps show up two to eight weeks after you contract the poxvirus that causes this skin infection. These initial bumps are small and firm to the touch and may appear in varying shades:
- Pink or reddish
- Flesh-colored
- Paler than your unaffected skin
Molluscum can show up anywhere on your body except for your palms and the soles of your feet.
2. Growing dome-shaped bumps
In the weeks after they appear, the lesions will grow into the shape of a dome, and a small, characteristic dent or dot will appear at the top of each lesion.
"The bumps will now have a small dimple in the middle, giving them a donut-looking appearance," says Dr. Amanda Stovall, a pediatrician at Springfield Clinic.
3. Spreading bumps
"Most often, bumps don't cause any symptoms. But sometimes they can itch, making it difficult to stop the spread," Stovall says.
While you might have a hard time not scratching itchy bumps, doing so can cause scarring. What's more, if you scratch the bumps and then touch the skin elsewhere on your body, you may end up spreading the virus to the rest of your body.
If you touch another person after scratching, you could also transmit the condition.
You may also experience large bumps or clusters of bumps at this stage, though this is more common if you have a weakened immune system due to an organ transplant, cancer treatment, or HIV infection.
4. Bumps about to clear
"As your body works to clear the infection, bumps may become red, dry, or flaky. This is referred to as the 'BOTE' sign, or the beginning of the end," Stovall says.
After several months, your bumps may turn red and resemble pimples. This means your body is fighting off the virus, and your lesions will clear up soon.
Keep in mind that as some bumps clear, new ones can pop up. This cycle often lasts 6 to 18 months before your skin clears and the virus goes away.
Diagnosis and treatment
Stovall says that molluscum usually clears over time without any treatment. "If your bumps are widespread or bothersome, a dermatologist can help," Stovall says.
Doctors can typically identify molluscum by looking at these bumps, but they may use a biopsy or scraping to confirm a visual diagnosis. Your primary care doctor might refer you to a dermatologist to discuss your treatment options.
Treatments include:
- Letting it clear on its own: If you have a healthy immune system, your body will eventually shed the virus, typically within two years.
- Antiretroviral treatment (ART): This treatment is recommended for HIV-positive people with molluscum daily to reduce the amount of the virus in your body.
- Cantharidin (beetle juice): Dermatologists have treated molluscum with juice from blister beetles since the 1950s. Your dermatologist will apply this to each bump across two visits to clear the skin.
- Curettage: A dermatologist pierces the core of each bump and scrapes out any material within. They'll repeat this treatment weekly until the bumps clear.
- Cryotherapy: Your doctor applies liquid nitrogen, an extremely cold substance, to each bump to freeze them off. Since new molluscum can still form, you'll return for treatment every 2 to 3 weeks until all of your bumps have cleared.
- Laser therapy: A dermatologist uses a pulsed dye laser (PDL) to remove bumps in under two minutes. While expensive, this treatment may be recommended if you have a weakened immune system.
"If the bumps are itchy, you can try an over-the-counter medication like hydrocortisone cream (avoiding face and genital regions, especially in young children) or oral Benadryl to help," Stovall says.
Complications
While this skin condition is usually harmless, it can cause some complications:
- Scarring from scratching or physical removal of bumps.
- Infections caused by bacteria entering an open lesion.
- Mental and emotional effects like poor mental health, low self-esteem, or relationship stress.
Kids vs. adults
Molluscum contagiosum is a common rash during childhood. This condition is mainly found in healthy kids ages 1 to 10, likely due to frequent skin-to-skin contact.
"Think contact sports, wrestling, and typical child play," Stovall says.
Still, it can affect people of all ages. You can acquire this virus by:
- Sharing clothes or towels with someone who has molluscum
- Touching an item someone with the virus has touched
- Swimming in contaminated pools or hot tubs
- Skin-to-skin contact like hugging or wrestling with someone who has molluscum
Teens and adults can also contract the virus from shared athletic equipment, like wrestling mats, and sexual activity.
Location of bumps
"Molluscum may be transmitted through sexual contact, so the lesions are more likely to be seen in the genital areas on adults and teens," Cody says.
Molluscum may show in different places on the body, depending on age:
- Children typically develop bumps on the face, trunk, arms, or legs.
- Adults may develop bumps on the genitals, lower abdomen, or inner thighs if the condition is sexually transmitted.
Treatment
"The rash tends to last longer in children, especially young children who can't help scratching and spreading it to different parts of their body or other people," Stovall says.
So, your dermatologist may recommend a certain treatment based on age.
Adults might have better self-control around scratching, so they might be better candidates for letting the virus run its course. Meanwhile, cantharidin is a common treatment choice for younger kids because it's quick and painless.
Prevention
Since molluscum is acquired through skin-to-skin contact, covering the rash with clothing helps you avoid transmitting it to others.
Other tips to help you avoid spreading it elsewhere on your body or transmitting it to others:
- Wash your hands regularly.
- Avoid shaving infected areas.
- Don't share or borrow personal items, including clothes, towels, and brushes.
- Avoid sexual contact, including kissing or touching affected areas.
- Use watertight bandages to cover bumps while swimming.
Insider's takeaway
Molluscum contagiosum is a common childhood rash that's typically harmless.
While the CDC says it's safe to send a child to school with molluscum, these bumps can still have a major impact on self-esteem and affect your relationships with others.
If you feel uncomfortable with letting this infection run its course or have concerns about transmitting it to others, a doctor can offer more information about your options for treatment.