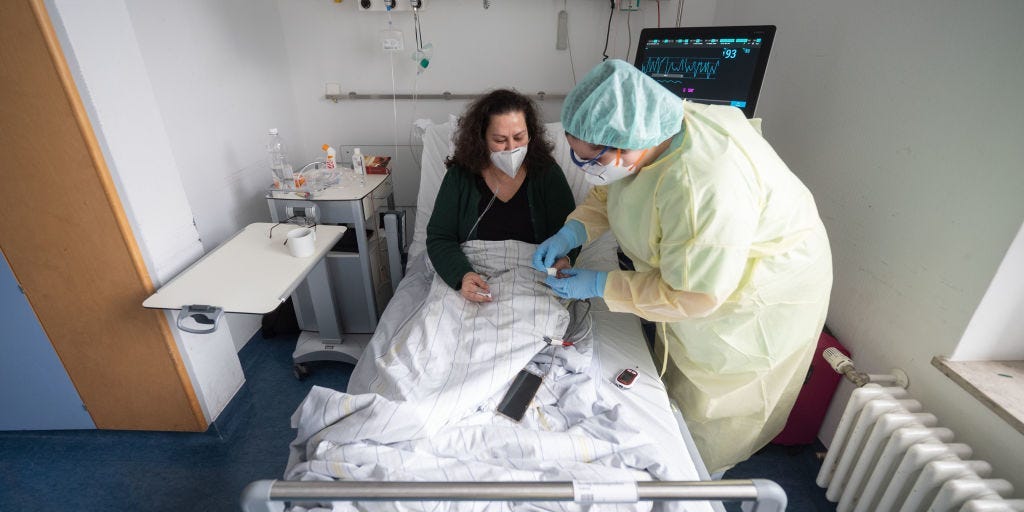
- Vicarious trauma is trauma a person feels indirectly, or vicariously, through another person.
- It is common among certain professions including healthcare workers, lawyers, and counselors.
- Vicarious trauma is usually a symptom of extreme empathy and in no way suggests you're bad at your job.
- Visit Insider's Health Reference library for more stories.
Vicarious trauma is a type of trauma that can cause mental health issues like post-traumatic stress disorder (PTSD) and depression.
As its name implies, vicarious trauma is trauma that a person experiences vicariously, or indirectly, through someone else.
"Vicarious trauma suggests that even though an individual may not have directly experienced or witnessed a traumatic event, it can still have harmful effects on them," says Timothy Schlairet, PsyD, of Thriveworks.
Vicarious traumatization is common among certain circles, but it is treatable. Learn how vicarious trauma can affect you, who is most at risk, and how to get help.
Symptoms
Psychologists often measure distress levels from vicarious trauma using the Vicarious Trauma Survey (VTS). The VTS was developed in 2008 to support professionals who work with traumatized clients on a regular basis.
The effects of vicarious trauma can appear in many different ways. You might:
- Have trouble trusting people after seeing the harm they're capable of
- Feel hopeless or depressed, like no matter how many people you help, nothing will change
- Avoid doing your job, whether through procrastination, tardiness, or distraction
- Feel irritated at nearly everyone and everything without knowing why
- Worry constantly about whether you are doing "enough" to help others
If you relate to any of these signs, know that you aren't alone. These are common responses to vicarious trauma. They don't make you any less professional, caring, or strong.
Who is most at risk?
Vicarious trauma tends to be most common among people in trauma-related fields such as:
- Mental healthcare: Examples include counselors and social workers
- Forensics: Examples includ lawyers and police officers
- Medical care: Examples include nurses, paramedics, and physicians
- Disaster relief: Examples include firemen and coast guard
These people often work to help the primary victims of trauma, and therefore are indirectly exposed to trauma as part of their job.
For instance, "many healthcare workers are experiencing vicarious trauma through the COVID-19 pandemic," says Lily Thrope, LCSW, of Thrope Therapy. "Watching people struggle to breathe is a really difficult thing to watch. Watching people struggle for their lives and not have any family members to comfort them is a trauma as well as a vicarious trauma."
Mental healthcare workers are also having problems. A 2020 study found over three-quarters of therapists had experienced "moderate" to "high" levels of vicarious trauma during the pandemic. These therapists felt less energetic, confident, and emotionally engaged in their work than they had before 2020.
However, you don't need to be in one of these careers to have vicarious trauma.
For example, racial and ethnic minorities who encounter violence against their communities can develop vicarious trauma, especially when graphic images or videos are involved.
Multiple studies on police violence against Black Americans show how potent vicarious trauma can be in the digital age. Police-related vicarious trauma can cause:
- Depressive episodes
- Hypervigilance
- Constant fear of death
- Dissociation
- Cynicism about the law enforcement system overall
Causes
"Vicarious trauma can be understood as a form of empathy mixed with anxiety," says Timothy Yen, PsyD, of Pivot Counseling. "When our brain connects with the pain and fear from another person and their situation, someone else's trauma can feel like it is happening to us too. That imaginative part of our brain creates the emotional connection of that fear, which is what contributes to the experience of vicarious trauma."
That's why, you are more vulnerable to vicarious traumatization if you have:
- Personal history of trauma
- Heightened empathy
- Trouble recognizing your own emotions
- Lack of support at work, especially training and debriefing
Related concerns
Vicarious traumatization (VT) overlaps with a few other conditions.
Post-traumatic stress
VT is, by definition, indirect. It only occurs when you have secondhand exposure to trauma.
On the other hand, PTSD can occur after any kind of trauma. You might be the primary victim, or you could witness a close loved one get hurt. Often you are personally involved in some way.
PTSD symptoms fall into four categories:
- Re-experiencing the trauma through flashbacks or nightmares
- Negative thoughts and feelings around trauma, such as blaming yourself for the incident or feeling "numb"
- Avoidance of trauma reminders, such as throwing away photos of someone involved in the incident or refusing to go into the building where the event happened
- Arousal after trauma in the form of insomnia, irritability, anxiety, and so on
People with VT can have many of these issues, but a PTSD diagnosis requires symptoms from all four categories.
Note that you can develop PTSD after vicarious trauma. In fact, research on homeless shelter workers shows people exposed to vicarious trauma have a higher risk of PTSD. Some people even believe that vicarious traumatization is a subtype of PTSD.
Secondary trauma
Research often treats vicarious trauma and secondary trauma as synonyms. However, there is some distinction:
- Vicarious traumatization emphasizes a change in thoughts. For example, you might become convinced that humanity is inherently selfish or aggressive. You could also grow more critical of yourself.
- Secondary traumatization emphasizes change in emotions and behavior. You could feel depressed or anxious. You might make lots of errors at work or find yourself having more arguments than before.
Compassion fatigue
Compassion fatigue is a kind of physical, emotional, and spiritual exhaustion. It often happens when you spend so much time caring for others that you neglect your own needs.
Vicarious trauma and compassion fatigue have quite a lot in common. In both conditions, you are likely to:
- Mull over stressful parts of your job off the clock
- Feel "drained," like you no longer have the energy to care
- Lose touch with your own sense of self
- Carry constant anxiety, irritation, or bitterness with you throughout the day
Unlike VT, you don't need to be exposed to trauma to get compassion fatigue. People in caregiving roles can get extremely stressed even if their day-to-day routine does not feel threatening.
Prevention
For some professionals, exposure to trauma is inevitable. However, VT is not.
Organizations can implement a number of risk-reducing measures to protect employees, including:
- Enforcing strong boundaries between work and home
- Debriefing after critical incidents
- Creating a robust supervision system for newer professionals
- Encouraging connection and cooperation between peers
- Destigmatizing rest and self-care
On an individual level, you can practice acknowledging and then filling your own needs. If you can recognize your VT symptoms early on, they may be easier to treat.
Treatment
What can you do if vicarious trauma has already impacted your mental health? You have a few treatment options.
Cognitive reframing
One common treatment method is cognitive reframing, an element of cognitive-behavioral therapy, which can help you change unhealthy patterns of thinking and behavior.
"For example, imagine a person is regularly hearing about car accidents in their occupation," Schlairet says. "It would be plausible that this person may begin to overgeneralize the frequency of car accidents. They may then begin to think that driving is entirely unsafe and also feel unsafe in a car."
"Although they may feel uncomfortable, that does not necessarily mean they are unsafe when driving," he adds.
In this scenario, cognitive behavioral therapy might introduce hard data to provide some perspective on how unsafe it actually is to drive a car. For example, the CDC WONDER system tracks the causes of mortality each year. The average person is twice as likely to die from poisoning as a car crash and roughly 15 times more likely to die from cancer.
Psychoeducation
Many interventions for VT include a psychoeducational element. This approach can teach you how to:
- Recognize vicarious trauma symptoms
- Reduce stress and increase mindfulness
- Develop a personalized self-care plan
Depending on your needs, psychoeducation interventions may last 1-12 sessions. They may be included with other treatment methods such as group therapy or stress reduction workshops.
A 2021 review of 27 studies found psychoeducation programs are often quite effective in reducing vicarious trauma symptoms. They can also reduce burnout, compassion fatigue, and anxiety.
Mindfulness interventions
The same 2021 review mentioned above also looked at five studies on mindfulness interventions, including yoga and meditation.
Participants in these studies reported improvement in cognitive and physical VT symptoms such as self-criticism and insomnia, respectively.
However, none of the studies had a control group, leading the researchers to conclude that more rigorous research may be needed before making conclusions.
Insider's takeaway
You don't need to be personally victimized to be impacted by a traumatic event. Vicarious trauma can have profound impacts on your well-being.
"Healing is an ongoing process and will require boundaries, mindfulness, and potentially a change in career, but it is possible," says Thrope. There is no shame in getting the help you need to feel better.









