- With the opioid crisis in full force and doctors feeling pressure to cut back on the number of opioid painkillers they prescribe, chronic-pain patients aren’t left with many alternatives that are as effective or accessible.
- So the pharmaceutical industry is looking to bring more non-opioid pain medications into market, with 17 drugs in late-stage clinical development and 40 drugs in early-stage development.
- One of the new types of drugs is used to block the nerve-growth factor, which can reduce pain in patients with osteoarthritis, chronic back pain, and cancer pain. The two newsworthy drugs in this category are tanezumab and fasinumab.
- Centrexion, a capsaicin-derived drug, has also received buzz for its pain-reducing properties.
Debbie Page, 66, has suffered from chronic pain for half of her life after a back injury left her with the inability to stand for more than a few minutes at a time.
“After an hour I can’t think or see,” she said. “The pain takes over and it’s torture.”
Page, a part-time occupational therapist in Boston, said oxycodone saved her life.
“I was at a point where I was seriously considering suicide or moving to Mexico. In trying everything, the only thing that ever has worked is opioids – ever,” she said. “They’re just magic.”
For many patients like Page, opioids are the only way they're able to manage chronic pain and lead full lives. Traditional nonaddictive medicine such as a class of drugs known as nonaspirin nonsteroidal anti-inflammatory drugs, or NSAIDs, does not work for everyone.
But with the opioid crisis in full force, doctors are feeling pressure to cut back on the number of opioid painkillers they prescribe, even among patients using them responsibly. This means the more than 100 million Americans suffering from chronic pain aren't left with many options that are as effective or accessible.
 Foto: source Shayanne Gal/Business Insider
Foto: source Shayanne Gal/Business Insider
For patients looking for alternatives to opioids, it can be hard to get them paid for by insurance companies. Treatments such as radio-frequency ablation, which uses radio-frequency waves to disrupts the ability of nerves to send pain, steroid injections and nerve-blockers, which are locally injected temporary anesthetics, are often labeled as "experimental" and "investigational" by insurance companies, effectively making them ineligible for reimbursement, despite being heavily recommended by many pain specialists.
So even when new technology, such as neuromodulation shows effectiveness, it can still be difficult for patients to get access to it. An increasing number of lawmakers are opening up to the concept of using marijuana as an opioid alternative, especially as a new study published in the Journal of the American Medical Association found that states with medical marijuana laws had lower opioid-associated deaths.
At the same time, drug companies and doctors alike are on the hunt for new ways to tackle the complexities of managing chronic pain. Some of the new approaches look to lifestyle fixes and cognitive therapies, while others look toward more medical-related interventions such as surgery and alternative medications.
'No doctor will take me'
There were more than 42,000 deaths in the US attributed to opioids in 2016, and 40% of all opioid-overdose deaths involved prescription opioids, according to the Centers for Disease Control and Prevention.
State lawmakers and some health systems, in turn, are putting measures in place to cap the number of opioid prescriptions that doctors dole out.
As a result, the number of opioid prescriptions nationally fell 22% between 2013 and 2017, according to a recent study from the IQVIA Institute for Human Data Science.
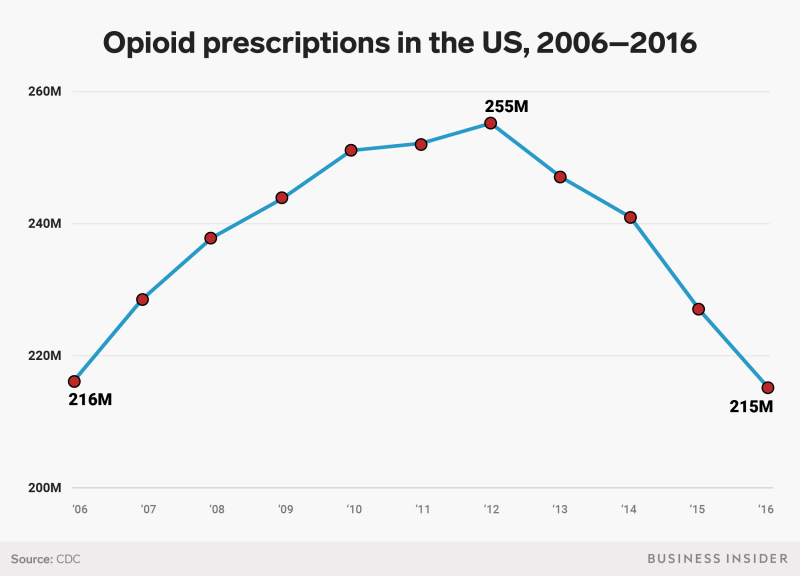
Page said she was already feeling the effects.
"I'm concerned every month ... no doctor will take me," she said. "I've had to travel three hours one day to fill my prescription. Everyone's out."
The problem is opioids are hard to beat when it comes to initial pricing, convenience, and immediate effectiveness.
Margaret Fitzpatrick, 52, was doing acupuncture daily to manage her chronic pain but had to cut back because the treatment wasn't covered by her insurance company after she exceeded 13 visits a year.
"Not having access to good therapists or acupuncture or massage is really frustrating especially with the opioid crisis and doctors not prescribing them when alternatives aren't covered by insurance," she said. Fitzpatrick was a teacher for many years, but had to stop working two years ago because of her pain.
"For those of us who are disabled, we don't have a lot of income, and you're taking away the alternatives that would work," she said.
For the most part, opioids work to reduce pain for a large number of people with different types of pain conditions, and there are usually minimal side effects if the patient has no history of substance-use disorder, said Cindy Steinberg, national director of policy and advocacy at the US Pain Foundation.
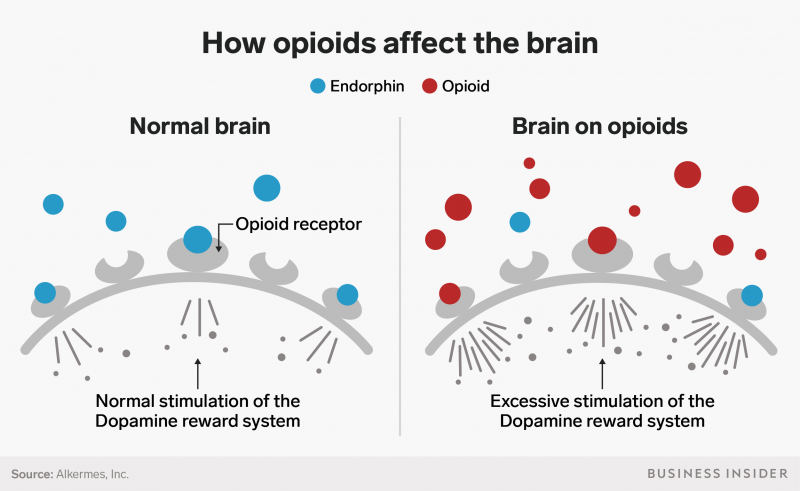
Opioids work by impersonating chemicals in the brain called endorphins, which act like messengers between nerve cells. The endorphin molecules bind to corresponding receptors on cells that exist in both the brain's pleasure center, and also on nerve cells that reside within the body's pain network.
These mock endorphins are far more potent than the natural ones produced by the body, so as they do their magic, they can elicit a wash of intense euphoria along with pain relief. But the body does become tolerant to this, and with every hit it needs more the next time to achieve the same response. Stopping entirely makes the body sick from withdrawal.
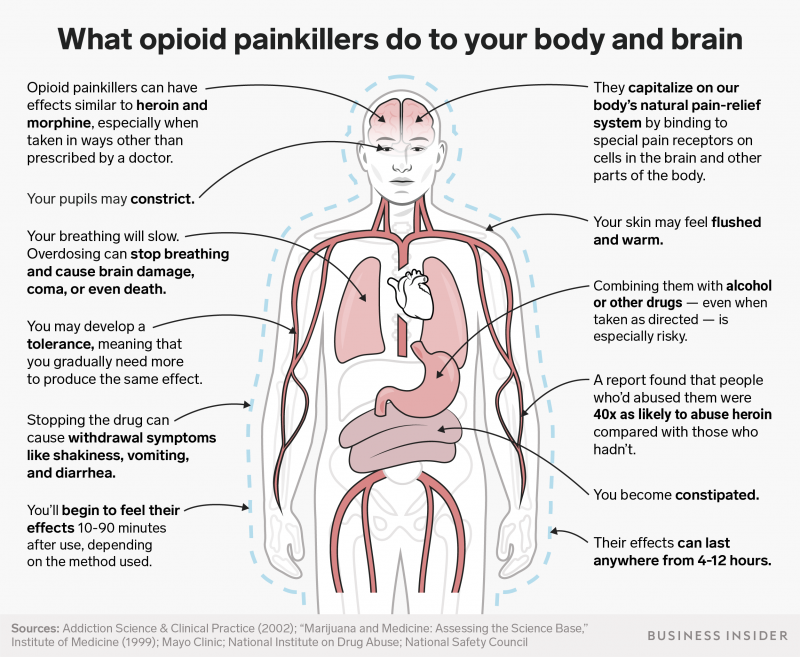
"Withdrawal is extremely painful," Page said. "I have to take the pill. The torture that people have to go through when they're suddenly reduced or kicked off is inhumane."
Finding alternatives
Dr. Janet Pearl, who runs a pain center outside Boston, described the pain she treats as a spectrum. Some types of anti-seizure medications and a class of antidepressants are effective at managing pain, while regenerative medicine is also an exciting area to tap into. For some patients, the body's wear and tear and genetics can make pain worse. For others, cognitive behavioral therapy works wonders. Patients need to be evaluated on a case-by-case basis, Pearl said.

Julie Morgenlender, a 39-year-old personal-finance consultant who's struggled with chronic pain for 20 years, has tried myriad treatments, including acupuncture, naturopathic medicine, and disease-modifying drugs like Plaquenil. She also suffers from autoimmune thyroid disease, for which she takes a drug called Nature-Throid.
"I have pain from each of these different things, and each one is just one piece of the puzzle," she said.
According to a Bio Industry Analysis published in February, pain accounts for a greater amount of direct US healthcare costs compared to diseases like cancer, diabetes, or cardiovascular dysfunction. Four times as many Americans suffer from chronic pain than diabetes.
Yet pain conditions are on the tail end of receiving venture funding. There are 11 unique types of drugs in the US approved for pain outside of opioids, easily eclipsed when compared to the 93 unique types of cancer drugs in 2017.
Pharma companies are just starting to invest more in drugs targeting chronic pain. There are 17 pain drugs in late-stage development to treat forms of chronic pain, as well as about 40 drugs in earlier human clinical trials.
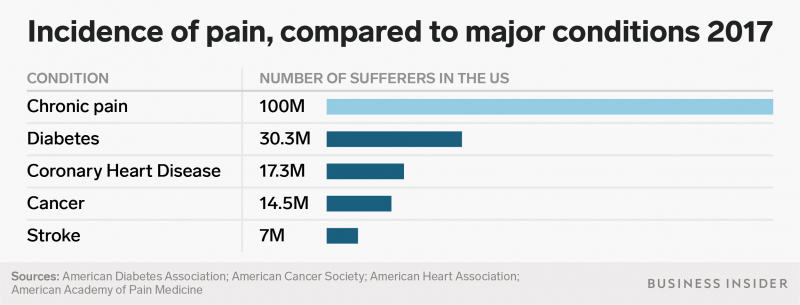
The types of formulas used to create pain medications needs to be expanded, and there needs to be wider discussion and increased legislation to provide access to these medications, said Neel Mehta, medical director of pain medicine at Weill Cornell.
"This is changing, but there was a time where if you wanted to use an alternative treatment, you had to establish failure of an opioids, purely because of cost," Mehta said.
One of the main approaches researchers are looking into is a class of drugs that work with nerve growth factor. NGF is important in developing babies' nervous systems, and they evolve to play a huge part in how adults feel pain.
"It stimulates peripheral nerves, and thereby you end up with a barrage of pain signals from the skin or muscles up through the body up through spinal cord into the brain where it's interpreted as pain," Ken Verburg, a senior vice president for development at Pfizer, told Business Insider. He's leading the development of tanezumab, one of the NGF inhibitors. Tanezumab blocks the effect of nerve-growth factor and lessens the sensation of pain.
The Canadian Agency for Drug and Technology in Health in February listed the approach as one of the emerging non-opioid drugs for management of chronic noncancer pain. It's one of the two major NGF-binding drugs that have surfaced in the pharmaceutical world.
- Pfizer and Lilly, tanezumab: In July, the drug said it had achieved its goal of lowering pain in a late-stage trial. It's used to treat osteoarthritis, chronic low-back pain, and cancer pain. Tanezumab was generally well tolerated, with approximately 1% of patients discontinuing treatment due to adverse events. Rapidly progressive osteoarthritis was observed in tanezumab-treated patients at a frequency of less than 1.5%
- Regeneron and Teva, fasinumab: A rival drug to tanezumab, it also targets low-back pain and osteoarthritis. Fasinumab was halted during its phase 2b trial in 2016, and in May, the company ditched the higher dosage of the drug. In mid-August, the companies announced positive results in a late-stage trial. Fasinumab was generally well tolerated. At week 16, 6% of the placebo group patients, 5% of the fasinumab 1 mg every eight weeks group patients and 6% of the fasinumab 1 mg every four weeks group patients discontinued treatment due to adverse effects.
While both tanezumab and fasinumab proved statistically signficant decreases in pain for patients in their late-stage trials, NGF blockers haven't always had a storied past. Fulranumab, an anti-NGF pain drug, was returned by Johnson & Johnson to Amgen in 2016 after a late-stage clinical trial because of safety concerns and has since been discontinued.
There's also a group of capsaicin-derived drugs that target the caspacin receptor (TRPV1) in the body to inactivate local pain fibers that transmit signals to other neurons. Capsaicin is a chemical extract from peppers. Repeated exposure to it cause substance P, a protein that transmits pain signals, to be used up, which reduces pain.
- Centrexion, CNTX-4975: In a phase 2 study, the drug kicked in within a few days and lasted about six months. "What our product does is it quiets down just the ends of pain fibers like giving a haircut," Kerrie Brady, chief business officer of Centrexion, told Business Insider in January. "And that stops the connection and stops the pain signaling going forward."
- Acorda Therapeutics, capsaicin 8% patch: It was approved by the FDA in 2009 to manage neuropathic pain. The patch is undergoing a late-stage trial with osteoarthritis patients.
Of the drugs in development, there are a couple of promising new candidates like Angiotensin II signaling that has a role in pathways of peripheral neuropathic pain, and EMA401, an old antagonist being repurposed by Novartis to treat neuropathic pain from diabetes.
Cornell's Mehta says that while these new drugs are promising, more needs to be more done about educating pain patients.
"Patients are open to it, but there are patients out there who are more apprehensive about it. We need to be cognizant of that. We need to do a good job of counseling, to be understanding of patient concerns, and encourage trials of other medications," he said. "We also need to understand with the new therapies coming in who is best suited for that."
Although Steinberg is waiting until all the clinical trials are done and the drugs formally enter the market, she holds out hope for the future of drug innovation in treating pain.
"If a drug can be as effective as opioids without the risk of addiction for those with substance-use disorder," she said, "it is worth the investment."
Lydia Ramsey contributed reporting.

