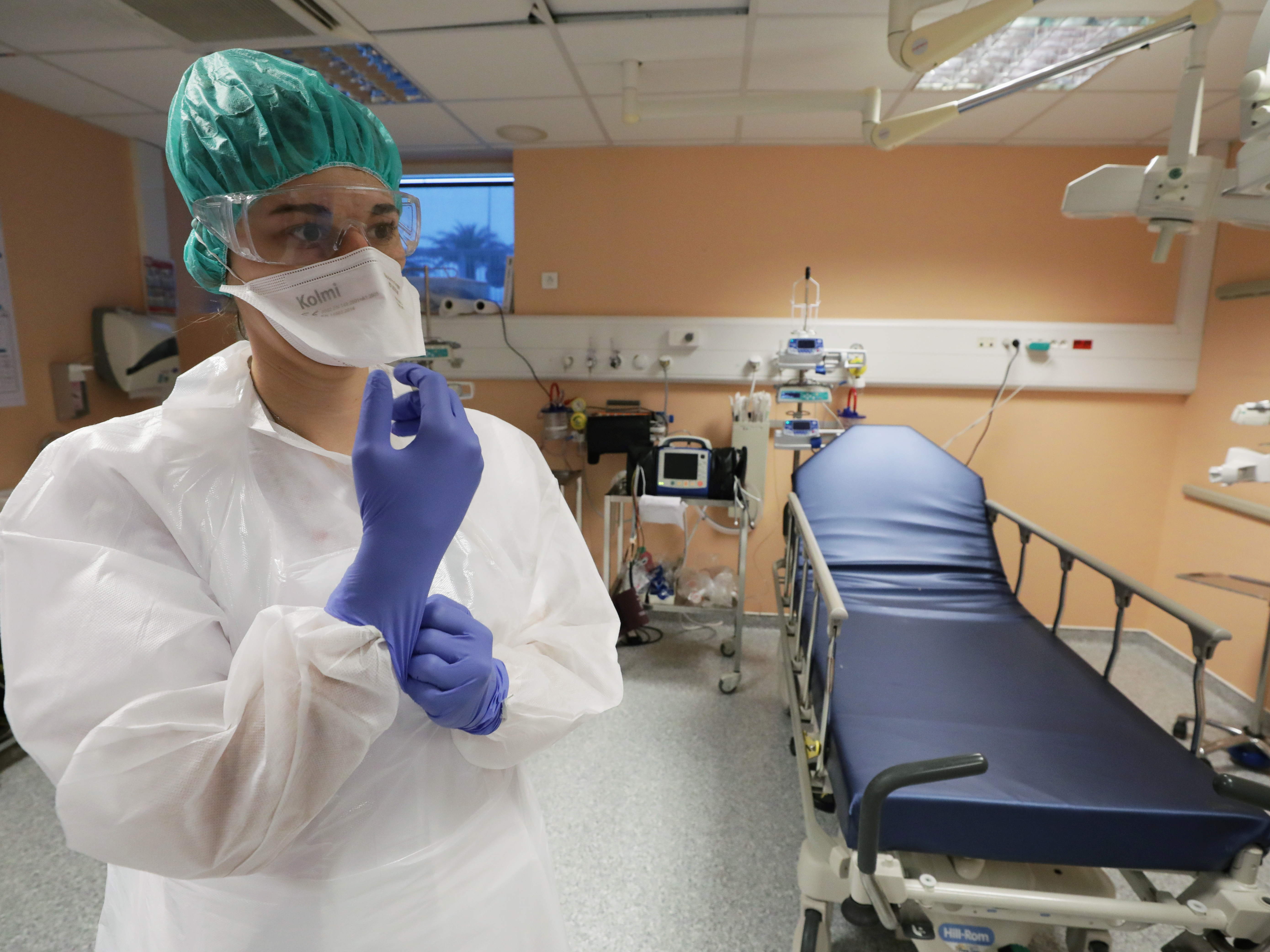
- Hospitals around the US are preparing for the novel coronavirus outbreak, which has sickened more than 200 people in the US and 100,000 worldwide.
- They want to make sure workers and equipment are ready to go in the event of a worst-case scenario.
- “We’ve not yet seen an epidemic or pandemic in our lifetimes of this size and scope,” said Becca Bartles, the executive director of infectious disease prevention at Providence St. Joseph Health System. “We’re gearing up for something extremely significant.”
- Visit Business Insider’s homepage for more stories.
When the first case of novel coronavirus showed up in the US in January, Becca Bartles was ready for it.
As the executive director of infectious disease prevention at Providence St. Joseph Health System, she had been preparing for years. Bartles helps prepare Providence, which runs 51 hospitals across the West Coast, for potential outbreaks by keeping an eye out for new pathogens that could hit the communities the health system serves.
“We’ve not yet seen an epidemic or pandemic in our lifetimes of this size and scope,” Bartles said. “We’re gearing up for something extremely significant.”
Hospitals and healthcare workers are already starting to feel the effects of the coronavirus outbreak as it hits communities around the US. The US has reported more than 200 cases of the novel coronavirus, which causes the disease known as COVID-19. More than 100,000 people have come down the virus worldwide, mainly in China.
And they're preparing for the outbreak to get worse.
Some of the hospitals Bartles works with are in the Seattle area and are already treating coronavirus patients. She said the virus is positioned to be the biggest outbreaks we've seen in recent US history.
'It will stretch our capacity to provide healthcare overall in the US' Foto: Becca Bartles, the executive director of infectious disease prevention at Providence St. Joseph Health System. Source: Providence St. Joseph Health
Foto: Becca Bartles, the executive director of infectious disease prevention at Providence St. Joseph Health System. Source: Providence St. Joseph Health
"I don't think we can appreciate, based on what we've seen in our lifetimes, how big that's going to be," Bartles said. "That does cause me significant concern."
"It will stretch our capacity to provide healthcare overall in the US," she added.
According to the US Centers for Disease Control and Prevention, reported symptoms related to the novel coronavirus include fever, cough, and shortness of breath, appearing within 14 days of exposure to the virus.
In a presentation hosted by the American Hospital Association, which represents thousands of hospitals and health systems, one expert projected there could be as many as 96 million cases in the US, 4.8 million hospitalizations, and 480,000 deaths associated with the novel coronavirus.
The American Hospital Association said the webinar reflects the views of the experts who spoke on it, not its own.
Preparing for the worst
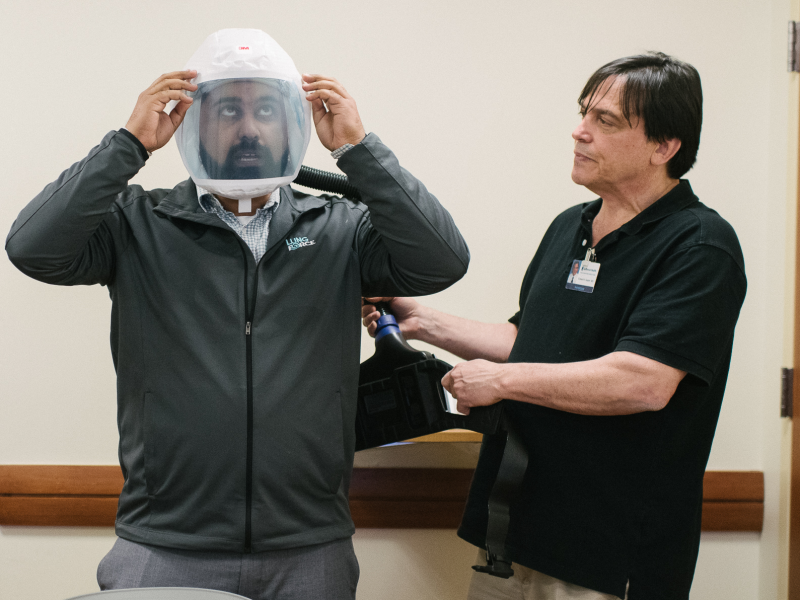
Health systems like Providence perform drills and trainings in anticipation of outbreaks like the novel coronavirus. The goal is to make sure employees, especially those working in the emergency department or who might care for critically ill patients, are trained correctly and have the right protective equipment.
And they're ramping those up now.
In Philadelphia, Jefferson Health has been conducting extra protective-equipment trainings, focused on intensive care unit clinicians who might treat people with the coronavirus.
The 14-hospital system also started a coronavirus task force this week and is readying its outbreak plans. The idea is to prepare for a worst-case scenario.
"We're saying, look, let's plan as if there's going to be a lot of cases, it's going to be overwhelming to our hospital," said Dr. Edward Jasper, an emergency medicine physician who leads the task force. "We don't think that's going to happen. And then whatever else comes, it's going to be nothing compared to that. So we're prepared."
For now, Jasper said he's not expecting the worst. "We watch it so closely and right now it's not triggering keeping me awake at night," he said.
At Providence, Bartles said leaders within the organization are now meeting multiple times a day to discuss issues like making sure the hospitals have enough supplies on hand, especially protective equipment for those working in emergency departments.
The goal of the meetings is also to inform other hospitals across Providence's network of what's going on in Washington, which has been hit hard with the virus.

How the largest health system in New York is preparing
The senior leadership at New York's Northwell Health System, which operates 23 hospitals, has been meeting continuously for the last several weeks, chief quality officer Dr. Mark Jarrett told Business Insider.
The discussions cover what happens if one individual comes in with symptoms all the way to a pandemic.
Northwell's relying on some of the preparation it did in advance of the SARS epidemic in 2003, and its response to the H1N1, or Swine Flu pandemic in 2009. But, Jarrett said, the hospital has changed a lot since then.
Northwell, New York's largest health system by revenue and the state's largest private employer, has been steadily moving more of its services outside the four walls of a hospital.
That means the health system will have to account for patients showing up for care in places other than the main hospital in a community - places like urgent care centers and primary care clinics.
Readying hospitals for a surge of patients
Should the outbreak intensify, hospitals are grappling with how to prepare for the surge in coronavirus patients while also keeping other patients safe.
At first, hospitals will isolate patients with the coronavirus, but if lots of patients come down with the virus, hospitals will probably put them in rooms together, said Kelly Zabriskie, Jefferson's director of infection prevention.
Dr. Kathleen Jordan, a vice president at CommonSpirit Health, a 142-hospital health system and chief medical officer at the system's Saint Francis Memorial Hospital, told Business Insider that the health system is having conversations about what might happen if they're confronted with an influx of patients.
That might include setting up tents, building out larger emergency rooms or adding more beds for patients who need to stay at the hospital. For now, the health system has a few cases of the novel coronavirus under investigation.
Eventually, hospitals might have to consider reducing or pausing elective procedures to make room for the surge in patients, Northwell's Jarrett said.
Hospitals are also thinking about staff being out, either due to the virus itself, or in the event that they have to care for their family.
Northwell on Tuesday told its employees that it's restricting travel for business both internationally and domestically through the end of March. That's a move other hospitals are making as well.
"These updated travel guidelines are designed to help us remain in good physical health so we can most effectively care for the patients and families we serve," Northwell said in an email to employees.
But you shouldn't rush to the emergency room if you start having flu symptoms.
Bartles said the plan is to focus on following CDC recommendations. As the virus continues to spread in communities, it will be harder to distinguish what might be flu from coronavirus.
Jan Emerson-Shea, a spokeswoman for the California Hospital Association, said hospitals are encouraging patients to call ahead or use an online doctor visit, rather than show up to an emergency room with potential coronavirus. That can help prevent them from infecting others, and let hospitals focus their resources on the most serious cases.
Bryan Pietsch contributed reporting.
- Read more:
- The US is sprinting to develop a coronavirus vaccine or treatment. Here's how 9 top drugmakers are racing to tackle an outbreak that's spreading around the world.
- 'Crazy hours, short nights': The inside story of how a buzzy biotech upstart developed a potential coronavirus vaccine in record time
- Gig economy workers say they'll have to work through the coronavirus outbreak even if they get sick: "We can't risk losing a day's income"
- Washington, California, and New York are forcing health insurers to cut patients' costs for coronavirus testing