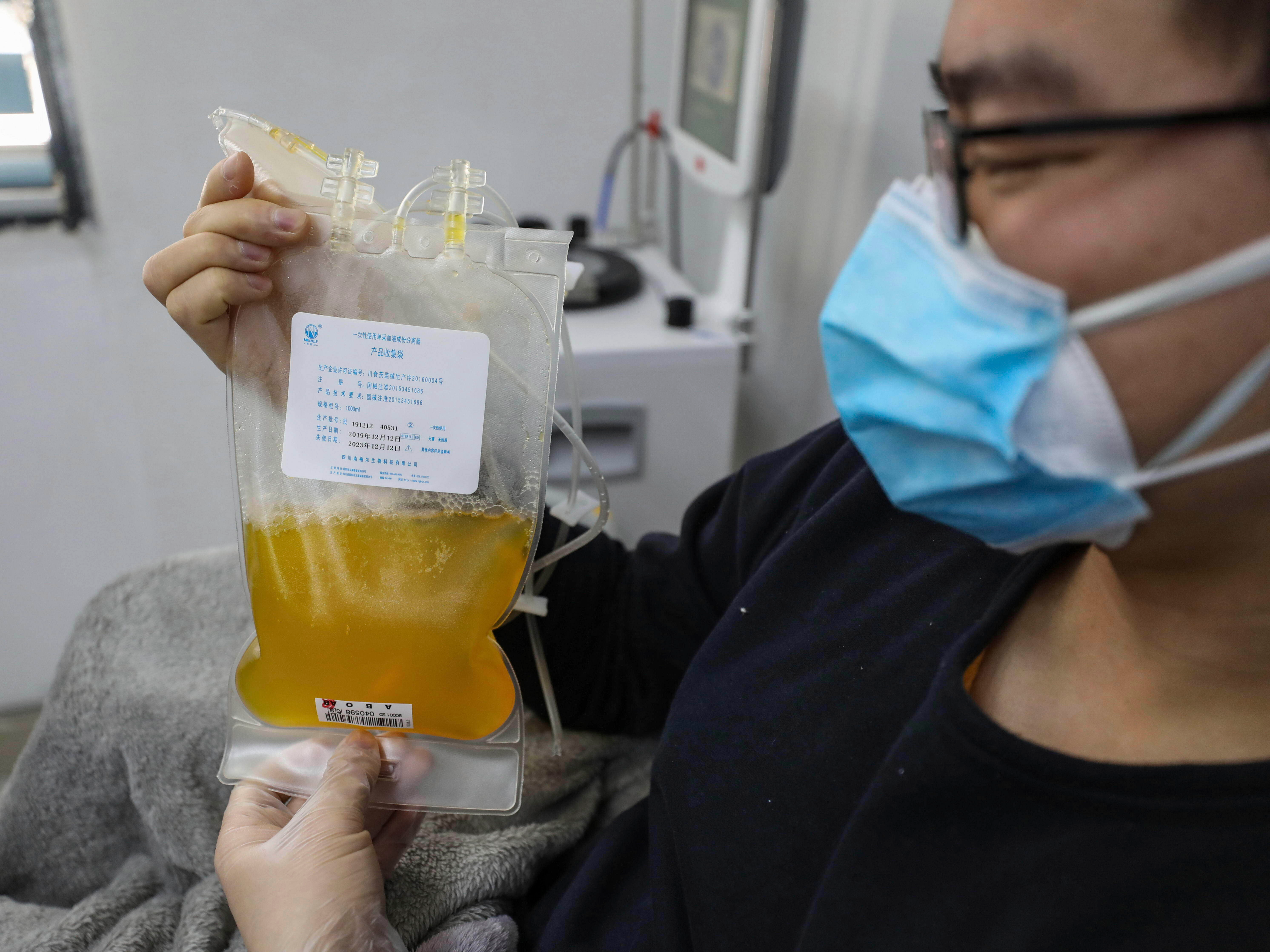
- Chinese researchers reported encouraging – yet early – results of a potential COVID-19 treatment.
- Five critically ill coronavirus patients got better after receiving an experimental treatment that’s made from the blood of people who’ve recovered from the virus.
- The early results were published Friday in the Journal of the American Medical Association, a leading medical journal. The researchers enrolled five COVID-19 patients with severe disease and transfused into them plasma from people who had recovered from coronavirus infections.
- The treatment, called convalescent plasma, is based on the fact that recovered patients have antibodies that can fight the coronavirus.
- The results showed the patients’ conditions improved after a transfusion. Three of the five were discharged from the hospital; the other two are still on ventilation but in stable condition.
- Visit Business Insider’s homepage for more stories.
A new report raises hope that the blood of recovered patients can help treat severe coronavirus cases.
Five critically ill patients were hospitalized in Shenzhen, China, with serious cases of COVID-19. They received an experimental plasma transfusion and have since recovered to varying degrees, according to new research published Friday in the Journal of the American Medical Association.
While the research is far too limited in size and rigor to draw conclusions from, the findings support more robust study of the treatment, called a convalescent plasma transfusion, the researchers concluded. New York announced this week plans to test convalescent plasma in severe cases of COVID-19.
Doctors conducted the study at a Shenzhen hospital from January 20 to March 25. The five patients, ranging in age from 36 to 73, received plasma between 10 and 22 days after being admitted to the hospital.
Within three days of the transfusion, four of the five had their body temperature normalize. Four of the five also saw their cases of acute respiratory distress resolve within 12 days.
All told, by the time the results were published Friday, three of the patients had been discharged from the hospital. The other two were both in stable condition, but still needed to be on ventilators in a hospital setting.
The study's limitations prevent big conclusions, but suggest potential
Along with the study, two Emory University experts, Dr. John Roback and Dr. Jeannette Guarner, interpreted the findings in an editorial for JAMA. Roback runs the Center for Transfusion and Cellular therapy at Emory's medical school, and Guarner is a professor of pathology and laboratory medicine.
They wrote that the five patient cases are "compelling and well-studied" but also limited. There was no control group in the study to compare the results against, they wrote, and five patients is a very small sample size.
Additionally, the patients were also receiving experimental antiviral drugs and steroids, which further limits the ability to pinpoint the effectiveness of the plasma transfusion.
Even with these limitations, the early findings raise the possibility of plasma transfusion as an effective COVID-19 treatment, particularly for critically ill patients.
"The results highlight the possibility that antibodies from convalescent plasma may have contributed to the clearance of the virus and also the improvement of symptoms," the Chinese researchers wrote.
Roback and Guarner wrote the findings support more rigorous testing in COVID-19. Similar plasma treatments have shown benefit in the past, with use during the SARS outbreak in 2002-03 and the H1N1 outbreak in 2009.
"If the results of rigorously conducted investigations, such as a large-scale randomized clinical trial, demonstrate efficacy, use of this therapy also could help change the course of this pandemic," the Emory experts said.
The potential treatment emphasizes the role of COVID-19 donors
Recovered COVID-19 patients provide the experimental treatment through blood donations. In the case of this study, the donors had all recovered from the coronavirus and reported feeling well for at least 10 days. Plasma was transferred into the patients the same day it was obtained, the researchers wrote.
If the treatment is proven to work on a larger scale, a critical challenge will be scaling up these donations to address a pandemic. Roback and Guarner said that blood centers could collect plasma from donors, and healthcare workers could encourage sickened patients to donate once they recover.
It also would be helpful to have antibody-detecting tests that could provide more specificity over time on which specific antibodies may be best, they wrote.